Project Description
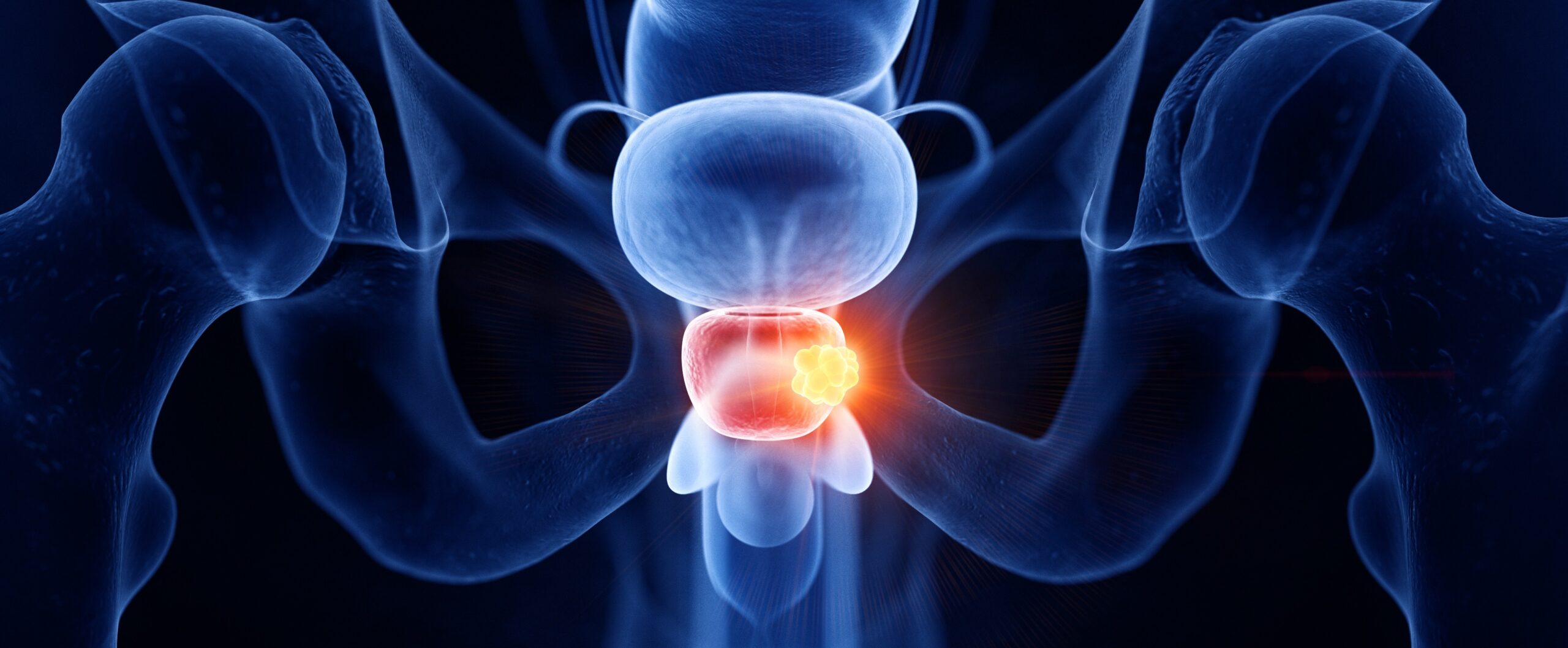
Prostate carcinoma is a common disease. Depending on the tumor stage, PSA value at the beginning of the disease (so-called iPSA) and Gleason score, patients are divided into groups with low, intermediate and high risk.
In principle, surgical procedures (radical prostatectomy with and without lymphadenectomy) and non-surgical procedures are used. When radiation therapy (radiation) is used, it is combined with antiandrogenic therapy for about 6 months (intermediate risk) or 24-36 months in the case of a high risk.
With a very different course and side effect profile, the treatment decision depends on the individual risk against the background of expectations of the therapy, possible side effects, limitation of quality of life, the question of incontinence and impotence risk, your age and co-morbidities. We offer you individual consultations, during which we take the time with you to find the most suitable therapy for your individual needs.
Various methods are used in the primary therapy of prostate carcinoma:
- External beam radiotherapy in a conventional fractionation (approx. 8 weeks of therapy);
- External beam radiotherapy in a conventional fractionation in combination with brachytherapy;
- the moderate hypofractionation, i.e. the reduction of the total treatment time from 8 to 4 weeks;
- the so-called ultrahypofractionation (e.g. as part of the Hypostat-2 study)
In the adjuvant situation after surgery, if risk factors are present, radiotherapy can be useful to reduce the risk of a PSA increase. For biochemical failure (PSA rising after surgery) a so called salvage radiotherapy is recommended.
The sooner radiation therapy is used, the more likely it is to cure. One therefore speaks of so-called early salvage radiotherapy at a PSA level of 0.2 ng/ml and of very early salvage radiotherapy at a PSA level of <0.2 ng/ml.
A PET-CT scan, which is mainly used in the case of an increase in PSA, supports us in making therapy decisions in order to uncover the cause of the increase (image).
MRI of the prostate is an important support when planning primary radiotherapy. By using it, the radiation volume can be kept as small as possible, since the CT tends to overestimate the size of the prostate.
Which documents would you ideally bring with you to our joint discussion?
- Punch biopsy findings (histology) with Gleason score, number of punches, number of affected punches,
- current PSA level and your past PSA levels
- MRI of the prostate
- If the PSA value is >10 ng/mg, a finding of whole-body skeletal scintigraphy or PSMA-PET-CT.
- Surgical report after radical prostatectomy with histological examination of the prostate and, if necessary, lymph nodes and
- resulting staging (e.g. pT2c pN1 (2/15) Pn0, R0)
- the address of your urologist and general practitioner
- If you have had radiation therapy before, please bring the radiation plans with you. We can advise you all the faster and more precisely at your first appointment as to whether further radiation therapy, to what extent, fractionation and dosage makes sense and is justifiable.
You can find more detailed information in the current German and American guideline.
What can you do to support the success of the therapy as much as possible?
- Please bring a shower or sauna towel with you to every radiation session.
- Please, be a little earlier to your appointments drink some water or tea in order to ensure optimal filling of the bladder.
- The bladder can best be spared if its filling level can be reproduced relatively well every day.
- A filling of 150-200 ml, which does not cause you any stress, would be optimal. After the irradiation, you will receive a measuring container in which you should urinate and write down the amount of urine. This gives you good feedback as to whether you can generate reproducible fillings. The technologists will ask you for the values.
- Avoid foods that cause gas, such as onions, garlic, legumes, peppers, fried/grilled or spicy foods.
- Check your weight once a week and record it, please.
- Make sure you have regular bowel movements. If you have problems (constipation such as diarrhea), please contact us.